


There’s something about March for me. It’s odd, it’s one of my favourite months because spring is on the way, the signs are everywhere. All around me life, nature, is preparing to break out from its long slumbers….For the most part, everything I see around me holds fresh promise, renewal, a celebration of this incredible world that happenstance brought to fruition.
Yet nature also exists inside of us, we are nature, though nature draws no great distinction between what we know as good and bad, it’s just nature. Earthquake, fire and flood are generally considered bad but we don’t blame nature for them. It’s the same with cancer. It’s entirely natural, that is to say, it’s of nature, it’s part of nature and it’s part of who we are.
So, in that sense, it’s hardly surprising that March seems to figure quite large in my various cancer journeys.
It was February 2012 when I finally got around to dragging my arse into a GP surgery to discuss my persistent, nocturnal cough, after 18 months of, well, forgetting mainly. It was March when I had the fatal diagnosis, the biopsies, the operation to remove the upper half of my right lung.
It was March, a year later, almost exactly, when I asked for an MRi scan of my head, fearing something but I didn’t know what. It turned out to be a lung cancer metastasis growing comfortably in the centre of my skull.
I’m now more than ten years past the first one and almost ten past the second. One of my current oncologists, I seem to have a collection, recently asked me to have another MRi of my brain. I asked why he felt that would be helpful. The truth is, he’s mainly just curious. He’s a leading Oncologist at two major London hospitals, at least, and they don’t have anyone who is ten years on from a brain metastasis.
When I was just six years on from the lung cancer, again in March, I was having a lovely meal in a restaurant in Westchester, New York with my brother-in-law, his wife, my wife and their mother who was 100 years old. As I write, she is still very much alive and still living in a care home in Westchester. My brother-in-law, Larry, is the former Medical Director of Phelps Memorial Hospital in Sleepy Hollow. He’s retired now but they asked him to stay on for a few years in a part-time capacity. He’s reputedly an excellent doctor. The restaurant was very nice, the food was good, the tables set with bright white linen cloths and napkins. So, when my nose started gushing blood, somewhat unexpectedly, the bright crimson stains were all the more shocking against the bleached white background. Shocked, I excused myself and headed to the bathroom to clean up.
When I returned, everyone had questions, unsurprisingly. Larry donned his “House” persona and began my interrogation. How long had this been going on? – Never, it’s never happened before. What other symptoms have you had? – Well, I have been getting these unexplained bruises, on various parts of my body. In fact I noticed a big one on my thigh when I stepped out of the shower, this morning.
When do you fly home? he insisted. We fly on Friday.
Well, tomorrow you’re coming to the hospital, we need to do some tests. I’ll set it up.
I spent the following day, all day, at Phelps. I had this test and that test including several blood tests. Eventually, having found nothing, except a large hole in my wallet, they let me go but made me promise I would arrange a stress-test ECG when I got home. I did exactly that, plus an angiogram of my heart, nothing. Apparently I was fit and healthy, except obviously something was wrong. Having exhausted all obvious avenues, I sort of resigned myself to it figuring that, sooner or later, some explanation would turn up. Except it didn’t.
When SARS-COV-2 arrived, IN MARCH, I spent a day in London doing a round of group meetings. Two days later I knew something was wrong and so I took myself to bed in the spare room where I stayed for nine days with a rather nasty flu, effluent emanating from every orifice; sweating, chilling, shivering, even hallucinations! I called the GP surgery on the second day, really just to speak to someone and make sure they felt I was doing all the right things: Temperature and blood oxygen monitoring, supplements (Vit-D, C, Questran, Zinc, Magnesium), lots of liquids and eating when I could (when I wasn’t throwing up).
I was ‘greeted’ by an answerphone message that said something along the lines of: “We’re closed, don’t you know there’s a ruddy pandemic on?! Where’s your social conscience?”. I’d heard that the government wanted us to phone 111 where we’d receive helpful, professional guidance. I called, about 9pm. I waited on hold for as long as my attention span allowed (about 30 minutes) with enormous effort, before collapsing exhausted. Later I thought, they might be less busy at two in the morning. I tried again. Same thing. I tried again at 3am. Same thing. I gave up. I figured, you’re on your own in this but that’s okay, you know what to do. Given my lung condition, however, had I started to get a bad cough, I’d already planned to drive myself straight to the Royal Brompton, the lung specialists, while I still could. In the end, I never got the cough, just the remaining smorgasbord of symptoms and a couple more thrown in for fun. At the end of the ninth day, I was weakened and enfeebled. I decided I needed to get gardening: fresh air, exercise and creativity. So that’s what I did and for the entire year I got more and more fit, my garden expanded by another six acres and a dozen or so maskless, unvaccinated, brave and sensible souls managed to earn a crust with me rather than sit on their arses going broke or exploiting furlough. No one got Covid.
However, my bruises hadn’t gone away and occasionally I was having nose bleeds. I decided I had to sort this out. I set a day aside and turned back to Mr. Google. I was about four hours in, all the articles concurred: a) I was senile and kept bumping my body without knowing/forgetting and b) I really shouldn’t pick my nose so aggressively.
I was just about to close one page when I spotted, in small print in the bottom left corner, the following short note:
“Of course, in some unusual cases, this could be a symptom of Lymphoma or Leukaemia.”
Oh.My.God.
The NHS was essentially closed, this was in late July, during lockdown. I now knew I was looking for a Haematological Oncologist and that was all I needed. I called several specialists in London, none would give a face-to-face consultation. How, pray, is a doctor going to diagnose me if he can’t examine me, for bruises, just say? And how does he take a blood sample via Zoom? I tried a different tack and found the Local Spire Hospital (not on my list of favourites) had a couple of such specialists listed and I looked them up. I chose one who was also, apparently, the senior consultant at the local NHS Trust and booked an appointment with him. On arrival I was obliged to give a PCR test and don a mask. The only such test and the only mask I have ever acquiesced to, or ever will again. I wasn’t yet determined enough and I very much wanted this consultation.
I met Gleb, nice man, kept his mask on (rules is rules) but didn’t blink when I removed mine upon entering the room. Gleb hails originally from Eastern Europe (Half Belarusian, half Ukrainian) and we had a fun talk about the state of things in Ukraine. This was 2020, of course, 18 months before the Russian incursion but right in the midst of the Kiev bombardment of Donbas and the East. He had a very interesting perspective, which we both shared. He had the nurse take a blood sample and process it while I waited and then he gave me his initial but fairly certain diagnosis. “I suspect you have a rare form of Leukaemia, CMML or Chronic myelomonocytic leukaemia for short.
He told me that he needed to take another, “special” blood test – one that had to be in a specialist lab within two hours – and, he explained, “This hospital has been taken over by the NHS, so I’m not sure what actually works any more”. He told me to go home and someone would call me to arrange the appointment. They did exactly that and, when the results came in, I went back for another consultation. Meanwhile, I had researched everything there was to be said on the topic of CMML. Rare, incurable, terminal. Can remain Chronic for some time but always progresses to ‘Acute’ or AMML, a bit like AML which is your common or garden variety of Leukaemia but one for which there is a bit more on the treatment front. I’d read that there had been some limited success with bone marrow transplants – for those who survived the process and the very few who went on to live a few years. I immediately determined, that was not for me. After surviving two terminal cancers without the need for aggressive chemotherapy, this would require extreme obliteration of my entire immune system, with all the attendant, debilitating effects. Not for me, I’m not that desperate to survive any more, having become somewhat inured to the concept of “death by cancer”.
I now knew the specific blood markers I needed to monitor to check my progress. I wondered why or how these had not shown up in the blood tests taken at Phelps, the results of which I’d never seen? Come to that, my local GP surgery subjects me to at least one blood test a year, how did they not spot it? The GP surgery never sends out blood test results, unless you make a song and dance but I had a sudden recollection on the short drive home. Earlier in the year, I’d made an application for a life insurance policy – half jokingly, as there was very slim chance they’d accept me, given my health record but, worth a try – I’d calculated it was the best and only guaranteed investment opportunity available at that time, at least for my wife’s benefit.
As part of that process, I’d been required to release my medical records and insisted that the GP send them to me, in the first instance. I recalled sighting several pages of blood test results and so I immediately rummaged in the filing cabinet, the instant I got home. I could hardly believe what I read:
16 Nov 2017 Monocyte count – observation; Platelet count – observation; Eosinophil count – observation;
05 Dec 2017 Ditto
28 Mar 2019 Ditto
27 Jun 2019 Ditto plus Reticulocyte count – observation
04 Nov 2019 Ditto
The word, “observation” is applied automatically by the laboratory, intended to draw the clinician’s attention and to suggest to them to investigate further. No one ever hinted there was anything wrong. No one called me or asked me to come and see a doctor. When I was having my nosebleed in Westchester, spending thousands of dollars for a day of examination at Phelps, driving myself slightly potty Googling to try to find answers, these idiots (the ones who put up the shutters at the first signs of Covid) had been sitting on the very answers I was seeking, all this time.
When I then received a message, asking me to attend an annual drug review at the surgery, the very exams that had resulted in these blood test results that were kept secret from me, I was so angry, I immediately dashed off an email:
“I’ve received a text from you asking me to book a non-urgent appointment for my annual drug review.
When I’ve attended these reviews over the last three years, I have my blood taken and it’s sent to the lab for tests. I’ve never once been given a copy of those tests results and aside from being told I should lose weight, no one noticed the blood cancer symptoms highlighted by the lab. Had they shared them with me, I would have taken action three years ago. They didn’t. Nor did they relate the flags to my medical history, where they would have seen that in 2013 I was subjected (at my request) to a very large dose of radiation in order to destroy a lung cancer metastasis in my brain. Radiation is one of the three causal factors (the only one that applies to me) of CMML. Yesterday I was diagnosed, by a Consultant Haematologist, with CMML. Median life expectancy 20 months. Starting three years ago. Yeah, thanks for that.
No, I can think of no sane or rational reason why I need another incompetent drug review. Can you?
Incidentally, given my short life expectancy, I doubt even a competent drug review would consider it humane to fail to authorise my repeat prescription for Hypertension and cholesterol medication.
Indirectly, I came by the attached blood test results earlier in the year, given an insurer requested a copy of my records. I have highlighted the flags the lab put on the high indications, to make it easy for you.”
…and I attached the pages referred to.
As I said, I was very angry.
Ten days later I received a letter from my long-standing GP of record (not that I had seen her very often) full of faux platitudes and suggesting I contact the Ombudsman! <stifled scream>
I replied:
“Dear Jill,
I’ve just received your letter, thank you. Frankly I was beginning to think my email of the 17th had fallen on deaf ears. I appreciate what you say but I fear I didn’t make clear the basis of my complaint. I’ll try to do better this time.
When I received my diagnosis, the previous day, I realised which were the key blood markers used to arrive at this conclusion. Recalling having seen blood test results, in the recently received extract of my medical records, I turned to these that morning. They date back to November 2017, four months prior to my having any symptoms, the ones that ultimately led me to seek out a haematologist/oncologist after years of being told there was nothing wrong with me.
Sure enough, there in that November blood test result, and every one of the subsequent results, my counts showed outside normal range. Above normal range, specifically. With almost every one, they increase, test on test. In each and every case, the lab’s software has flagged each one as above normal range and, in each case, applied the alert: “Observation”.
Jill, I’m a very busy guy but I can tell you, with absolute conviction, that I would have been onto this like a shot, had I been aware of it. Not only did no one take the time or trouble to contact me, heaven forbid I should be sent a copy of *my results as a matter of course, but no one, clearly, bothered to read them. I refuse to believe that a competent doctor, that is to say, a non-negligent doctor, would have read those results, seen the word “Observation”, repeated so many, many times and fail to act in any way, shape or form.
I’m aware that the standard instruction is to “call the receptionist” if you want to know the results of your blood tests. It’s always infuriated me. On occasion, I’ve actually done it and the response to my question has always been “All fine, if there was anything to be concerned about the doctor would have contacted you.” Really?
I don’t pay the enormous sums I’ve paid over my life to ask a receptionist to diagnose leukaemia, that’s what we pay doctors for. If I have the information, then at least I’m a second line of defence but keep that information from me and the entire responsibility lies with the assigned doctor, if there even is one in the case of my “annual review” blood test results.
I wouldn’t even blame the average GP for not spotting the indicators for an extremely rare blood cancer, even though they are similar to other blood cancers. However, when the patient in question has already had two bouts of cancer, I might look a little closer, if I were him. If the lab had done the heavy lifting for me and flagged the symptoms with clear wording, over multiple test results spanning at least a three year period, it wouldn’t have bypassed me.
According to everything I read, and my specialist, the median life expectancy for CMML is 20 months. You can understand that I’m just a little pissed off that the information confirming my condition has been sitting on my file for 36 of those 20 months unnoticed and unheeded. Let’s hope I can continue to buck the trend for a tad longer, I’ve got rather a lot to do, in a rather truncated space of time.
I want to make myself clear. I’m not blaming anyone at the surgery for my condition, I am, however, literally sick to death of paying people to do a job of work for which they are either patently unqualified, hopelessly inadequate or frankly incompetent to do to an acceptable standard. I am sick of a state imposed health service that is frankly more adept at leaving people to die, than it is at making them well. I don’t want to use the NHS, ever but it insinuates itself into my life in ways that I am hamstrung to avoid.
By way of a further example, when I was racked with fever from CV19 at the end of March, early April, I took care of myself for the nine days of my vile sickness. I’ve got no problem with that, I just needed to be able to talk to a doctor to make sure I was doing all the right things. I called the surgery which went straight to answerphone. Now I accept that I’m paraphrasing here but my recollection of the message was: “Don’t you know there’s a pandemic on? Sod off!”. Seriously.
Oh, yes, I did call 111, three times actually, on different days at different hours including 3am once. When you’re feeling fit and well, it’s tediously frustrating to be told, every ten seconds, that “your call is important to us” but when you’re sick and exhausted, I could only take thirty minutes of it before hanging up. On one of those occasions I actually dozed off, that was nice.
On the matter of hospital reports, my consultant Gleb Ivanov has twice written to you, cc to me, with details of my two consultations. Yesterday I had a BMB at his hands, quite the most excruciatingly painful thing I could even imagine. I mention this because you raised the matter but again, I emphasise, it’s not treatment, I’m lacking, it’s faith in your GP surgery, let alone the NHS.
Yes, in the vain hope that my experiences might help drive even a modest improvement in the quality of care your patients receive, do please record this as an official complaint. Just excuse me if, after 67 amazing years on this planet, I don’t hold my breath for any outcome at all before I die, let alone a beneficial one.
You might have noticed, I’m a tad cross. At least I will have achieved something, if that has registered.”
While this sideshow was rumbling, at the subsequent consultation Gleb had delivered the confirmation and the prognosis. Not good. He asked me if I’d agree to a bone marrow “aspiration and trephine biopsy”. Basically a core sample of bone and marrow taken from my the top of my hip bone, at the rear, with local anaesthetic…..I agreed and after it was over, determined I would never have another so long as I live. It was the most excruciatingly painful experience of my life.
Meanwhile, I had tracked down an expert in my disease, Professor John Gribben. I met with him and he reviewed all the data, concurring with Gleb on the diagnosis, along with the “watch and wait” strategy (given the absence of treatment) but differing in the prognosis. “I think you have many years.”, he declared. That was, without question, the best news I’d had in a long time. I asked him if there was anything I could do to help my body fend things off as long as possible. “Avoid stress”, he intoned. A man of few words and I really like that. Unfortunately, I’ve had no success in following his advice.
Gleb organised a “molecular screening” where my DNA was tested in order to properly model my disease stage/prognosis, according to the latest tools and to have it available in case any “targeted therapies” became available. Aside from that it was generally agreed that I have regular blood tests every three months to monitor my markers until such time as the disease progressed to AMML. And so we did exactly that.
In September, last year, 2021 someone told me that, as a gardener, I should watch a little movie documentary on Amazon Prime called Fantastic Fungi, featuring one Paul Stamets who is, to say the least, something of a mushroom guru. It’s a fabulous film and you should watch it for many reasons. I loved the entire thing, there are many facets but my attention was also caught by reference to the use of mushrooms as a treatment/supplement with benefits for cancer. This sent me on a little journey. Paul has a TED talk on YouTube where he explains the situation with his 80 y/o mother who was diagnosed with “the worst case of stage 4 breast cancer” the oncologist had ever seen and given three months to live. In combination with her chemotherapy drugs, which were not thought to be able to halt the cancer’s progression, given her age and the stage of metastasis, she took Turkey Tail mushroom extract. One year later, she was declared “cancer free”. That’s the nearest one ever gets to the word “cured” when we’re discussing cancer. Remarkable.
I read article after article, study after study. I don’t go in much for hippy-dippy cancer cures, as some of you will know but this one I couldn’t ignore completely. There were practical, chemical reasons why it just could be effective. I decided to give it a try.
I wanted to make sure that I was doing so in as controlled an environment as I possibly could. I had stopped taking Statins about the same time – for entirely different but equally well-researched reasons – and I didn’t want this to confuse what might be seen to be going on in my blood, no matter how improbable. Thus I waited until I’d had my routine blood test, the following June 2022. Now I had a baseline to measure from. No Statins for nine months, no other changes to medication or anything else of note.
In June my Monocytes were not at their highest (3.3) but near it at 2.9 – the normal range is 0.2-1.0. That evening I started to take my Turkey Tail capsules, four in the morning and four at night. I didn’t tell anyone involved in my medical care.
My September blood test was cancelled and when it was reinstated, it was for 7th November 2022. It was annoying and suspenseful but I reasoned that a five month test could only be better than my intended three month one, anyway – aside from costing me in more mushroom extract if, as I suspected, it was going to prove worthless.
Gleb and I had our usual ten minute discussion on the faults of the Ukrainian people, in Gleb’s eyes, much of which I sympathised with and then he casually murmured, “Well, let’s see, your monocytes are back within normal range, your neutrophils…..they’re within normal range…..your….. I was gobsmacked! He made no real comment other than, “So that’s good…..”
Genuinely a little stunned and, frankly, not believing what I was hearing, I asked if he could print me a copy of the results. “I would”, he said, “but this printer is broken.” I tell you what, come with me and I’ll get the secretary to print one for you.”
We walked out of his office and across the waiting room to where the admin and nursing staff in Phlebotomy hang out and, sure enough, I was given my printout. We shook hands and I parted, desperate to get back to my car so I could read the report carefully. There it was, in black and white – all my markers well within normal range. All of them! Except platelets, for some reason, I have to keep an eye on that but that’s another thing entirely.
Was the lab machine broken, like his printer?
Had they mixed my blood sample up with someone else’s? Someone who, as I was reading my good news, was being given the worst possible bad news?
I need another blood test to confirm, don’t I? This can’t be true. The results just could not be this good. It’s a ruddy mushroom, for Pete’s sake! Now this you might find a little nerdy, sad even, but I have been keeping a running spreadsheet of my blood results going back to 2016. I do this partly because no one else involved in my medical care does it. How they can do their job properly I don’t know. I also do it so I can get early warning of things that might be going awry and because of all the different result formats I get given with differing amounts of data. My spreadsheet illuminates and presents a graphical image of my descent/progress.
When I got home I plugged in the numbers. If you think keeping a spreadsheet is nerdy, then let me confess it includes the normal ranges for each marker and the number in question appears either in black type (within range) or red (outside normal range).
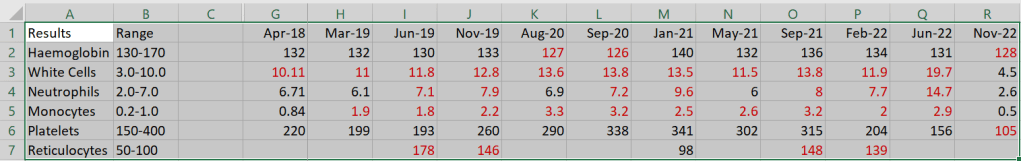
My haemoglobin has always bounced around the min level, all my life, so I’m unconcerned about that. Why my Platelets have fallen off a cliff is a mystery but we’ll look into that, but just look at the collapse in White Cells, Neutrophils and Monocytes! That’s incredible. I’m actually below where I was in December 2016.
I was still trying to let all this sink in when I suddenly remembered, I’d had an annual medication review in October, just three weeks previously. As usual, the surgery never gives you a copy of the report or tells you how it went BUT I do now have them uploading my results to their “system” so I can access it via an app. I grabbed for my phone and opened it up…and there was my confirmatory blood test, the one I felt I needed to rule out the possibility of a mistake:
White Cells: 7.7 Normal Range
Neutrophils: 3.9 Normal Range
Monocytes: 1.0 JUST in Normal Range!
In short, my numbers in November were even better but that was at the end of a progressive decline over the previous five months (and in another sense, over six years!).
So, do I now believe that Turkey Tail mushrooms “cure cancer”? Well, they certainly make it one heck of a lot better.
The final proof would be another Bone Marrow and Trefine aspiration but that ain’t going to happen, watch my lips. The fact is that, right now, if I went to a Consultant Haematologist and asked if I had cancer, he would say “No”. Is that a cure? Will they turn upward again? What if I stop taking my “magic” mushrooms, what then? All of those questions are currently unanswerable but am I more optimistic than before? Absolutely.
I requested a call with Professor Gribben and it was set up for a Monday late afternoon. It never came because the poor Professor was so busy he didn’t get through his other calls until 10pm so it was not to be. We rearranged for the following week, it was torture. I had burning questions I wanted to ask and I had emailed him my spreadsheet and the two most recent blood tests. So it was, Monday 21st November. Despite driving back from an engagement as fast as I could and getting home 20 minutes ahead of the call so I could be calm and prepared, I discovered the Broadband was down and my network in a mess. It was blowing a gale outside, cold and raining but it was the only place I could get a phone signal. I waited over half an hour but eventually he came on.
“So, he began, I’ve read your spreadsheet and the other reports, this is amazing! What have you been doing?!”
Not wanting to influence the conversation, I asked “Is it? Is it really amazing? I thought you were going to tell me, yeah this kind of thing goes up and down all the time, nothing to get excited about.”
“This NEVER happens, he replied, it is amazing, what have you been doing?”
“Well, I started cautiously, I didn’t want you to think I was some kind of nutter but the thing is, I’ve been taking these mushrooms…..” and I went on to describe the specifics. “This could make you and I rich!”, he exclaimed but tongue in cheek, obviously.
We chatted a bit and he promised to organise another blood test through my GP, on the premise of investigating the drop in Platelets, which would give us even more solid confirmation – or something else. He did exactly that and, at the time of writing, I’m awaiting an appointment for January. That’s the thing about cancer, you spend most of your time waiting.
Waiting and wondering and daring to hope.
